Current Concepts in Rehabilitation Following Ulnar Collateral Ligament Reconstruction. Initial Postoperative Management. The athlete is often placed in a posterior splint, with the elbow immobilized at 9.
This allows preliminary healing of the UCL graft and soft tissue slings involved in the nerve transposition. Close monitoring of the ulnar nerve is recommended. The patient is instructed to perform wrist active ROM and gripping, as well as submaximal multiple angle isometrics for the wrist and elbow. One consideration for early postoperative rehabilitation is based on the surgical approach and condition of the flexor pronator origin. The figure of 8 involves the complete detachment of the flexor/pronator origin from the medial epicondyle. Care must be taken not to perform active wrist extension during the initial 6 postoperative weeks. The modified Jobe procedure utilizes a muscle- splitting approach that does not interrupt the flexor/pronator origin, thereby allowing more aggressive early ROM of the wrist and forearm, as well as the initiation of the submaximal isometric exercises.
Knowledge of the surgical approach is important to guide the early ROM and resistive exercise progressions. The patient is progressed from the posterior splint to an elbow ROM brace at 7 days postoperative to initially allow 3. Motion is increased each week by 5. Full passive range of motion (PROM; 0. The brace is discontinued between week 6 and week 8 in most patients. A more rapid return of PROM with acute UCL injuries may be appropriate, with full PROM by week 5 or week 6. For the chronic tears, full PROM is restored more slowly, usually 6 to 8 weeks, postoperatively.
Recent research by Bernas et al (unpublished data, 2. UCL (gracilis graft and docking procedure) during PROM. Simulating early rehabilitative stressors in cadaveric UCL reconstructions, PROM between full extension to 5. In addition, forearm rotation (supination and pronation) has no effect on graft strain. Simulated isometric muscle contractions had no effect on the strain in the UCL reconstructions.
The UCL graft and the fascial slings, which stabilize the transposed ulnar nerve, are protected by gradually progressing elbow extension to 3. Wright et al. 30 reported that the average loss of elbow extension was 7. Furthermore, Ellenbecker et al. Directly related to elbow function was wrist flexibility, which was significantly less in extension on the dominant arm because of tightness of the wrist flexor musculature. There was no difference in wrist flexion ROM between extremities. If the patient has difficulty achieving full extension after UCL reconstruction using ROM and mobilization techniques, a low- load, long- duration stretch may be performed.
ULNAR COLLATERAL LIGAMENT. Week 1 Brace: Posterior splint at 90 degrees elbow flexion Wrist AROM ext/flex. Ahmad POST UCL RECONSTRUCTION PHYSICAL THERAPY PROTOCOL 2. 06/01/04 Ulnar Collateral Ligament Reconstruction of the Elbow Rehabilitation Protocol Methodist Sports Medicine Center, Indianapolis, IN Department of Physical Therapy A longitudinal incision is made beginning along the. Injuries to the ulnar collateral ligament. NCBI > Literature > PubMed Central (PMC). What Are Ulnar Collateral Ligament. This ligament helps to support and stabilize your. Have you had to stop playing your sport because of the injury to your elbow? Your physical therapist may gently poke around your.
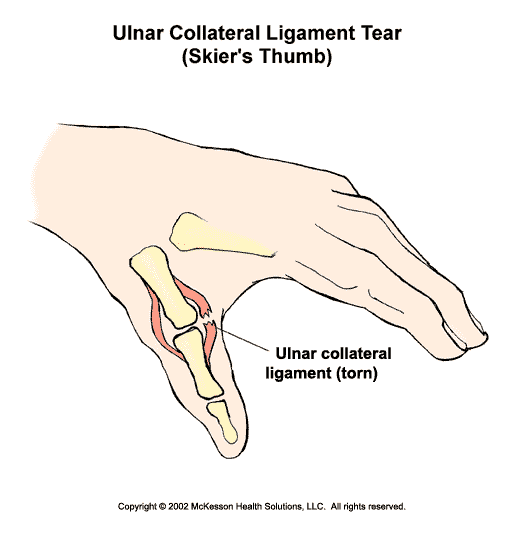
The most common symptom of a torn ulnar collateral ligament elbow injury is pain on. What causes ulnar collateral ligament (UCL) injuries? The ulnar collateral ligament can become stretched, frayed or torn through the stress of repetitive throwing motions. If the force on the soft tissues is greater than the. Physical Therapy in Boston, Medford and Wellesley for Elbow. Welcome to Orthopedic & Sports Physical Therapy / Advanced Sports Therapy's patient resource about Ulnar Collateral Ligament Injuries. The ulnar collateral ligament.
This technique can be extremely beneficial for regaining full elbow extension. The patient lies supine with a towel roll or foam placed under the distal humerus to act as a cushion and fulcrum. Light- resistance exercise tubing is applied to the wrist of the patient and secured to the table or a dumbbell on the ground (Figure 1). The patient is instructed to relax as much as possible with the arm in full extension and in forearm pronation for 1.
The resistance applied should be of low magnitude, to enable the stretch for the entire duration without pain or muscle spasm (ie, low load, long duration). Patients perform the low- load, long- duration stretches several times per day, totaling 6. The total end- range time program.
A low- load, long- duration stretch into elbow extension, performed using light resistance. The aggressiveness of stretching and mobilization techniques is dictated by the healing constraints of involved tissues, the pathology/surgery, the ROM, and the end feel. If the patient presents with a decrease in motion and hard end feel without pain, aggressive stretching and mobilization technique may be used. Conversely, a patient with pain before resistance will be progressed slowly with gentle stretching. Rehabilitation of the postoperative elbow should include proprioceptive exercises. Angular replication and end- range reproduction exercises can be used early in rehabilitation to stimulate mechanoreceptors in the postoperative joint.
Loss of kinesthetic awareness of the upper extremity can occur following injury. Manske et al. 14 found decreased proprioceptive acuity in the dominant elbows of college- level baseball pitchers after simulated throwing for 3 innings. The total arm- strengthening concept should be followed during rehabilitation after UCL reconstruction. Emphasizing proximal scapular stabilization early in the rehabilitation program and continuing this emphasis using a low- resistance, high- repetition program restores the necessary proximal stabilization to promote an optimal return to uncompensated throwing. This includes scapular stabilization via manual resistance to elicit serratus anterior and trapezius/rhomboid muscle activation without compromising the repair.
Physical Therapy in Boston, Medford and Wellesley for Elbow. Introduction Welcome to Orthopedic & Sports Physical Therapy / Advanced Sports Therapy's patient resource about Ulnar Collateral Ligament Injuries. The ulnar collateral ligament (UCL) can become stretched, frayed or torn through the stress of repetitive throwing motions. Professional pitchers have been the athletes treated most often for this problem.
Javelin, football, racquet sports, ice hockey, and water polo players have also been reported to injure the UCL. A fall on an outstretched arm can also lead to UCL rupture (often with elbow dislocation). This guide will help you understand: how the problem developswhat causes this conditionhow doctors diagnose the conditionwhat treatment options are available. Anatomy. What parts of the elbow are affected? The bones of the elbow are the humerus (the upper arm bone), the ulna (the larger bone of the forearm, on the opposite side of the thumb), and the radius (the smaller bone of the forearm on the same side as the thumb). The elbow itself is essentially a hinge joint, meaning it bends and straightens like a hinge.
But there is a second joint where the end of the radius (the radial head) meets the humerus. This joint is complicated because the radius has to rotate so that you can turn your hand palm up and palm down.
At the same time, it has to slide against the end of the humerus as the elbow bends and straightens. The joint is even more complex because the radius has to slide against the ulna as it rotates the wrist as well. As a result, the end of the radius at the elbow is shaped like a smooth knob with a cup at the end to fit on the end of the humerus. The edges are also smooth where it glides against the ulna. There are several important ligaments in the elbow. Ligaments are soft tissue structures that connect bones to bones. The ligaments around a joint usually combine together to form a joint capsule.
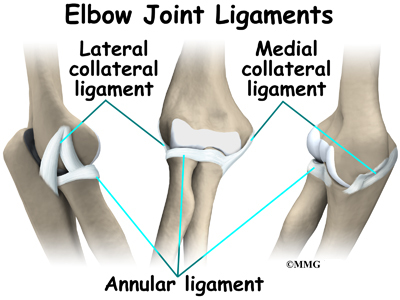
A joint capsule is a watertight sac that surrounds a joint and contains lubricating fluid called synovial fluid. In the elbow, two of the most important ligaments are the ulnar collateral ligament (UCL) and the lateral collateral ligament. The UCL is also known as the medial collateral ligament. The ulnar collateral ligament is on the medial (the side of the elbow that\'s next to the body) side of the elbow, and the lateral collateral is on the outside. The ulnar collateral ligament is a thick band of ligamentous tissue that forms a triangular shape along the medial elbow. It has an anterior bundle, posterior bundle, and a thinner, transverse ligament. Together these two ligaments, the ulnar (or medial) collateral and the lateral collateral, connect the humerus to the ulna and keep it tightly in place as it slides through the groove at the end of the humerus.
These ligaments are the main source of stability for the elbow. They can be torn when there is an injury or dislocation of the elbow. If they do not heal correctly the elbow can be too loose or unstable. The ulnar collateral ligament can also be damaged by overuse and repetitive stress, such as the throwing motion. Related Document: Orthopedic & Sports Physical Therapy / Advanced Sports Therapy's Guide to Elbow Anatomy. Causes. What causes ulnar collateral ligament (UCL) injuries? The ulnar collateral ligament can become stretched, frayed or torn through the stress of repetitive throwing motions.
If the force on the soft tissues is greater than the tensile strength of the structure, then tiny tears of the ligament can develop. Months (and even years) of throwing hard causes a process of microtears, degeneration, and finally, rupture of the ligament. The dominant arm is affected most often. Eventually the weakened tendon my rupture completely causing a pop and immediate pain. The athlete may report the injury occurred during a single throw, but the reality is usually that the ligament simply finally became weakened to the point that it finally ruptured. However, the general profile associated with this injury may be changing.
Today, more and more children ages 1. Longer seasons with extended practice time and more tournaments increase the risk of UCL injury. Throwing volume, pitch type, and throwing mechanics can all contribute to the problem. Children have their own unique risk factor in that they have an open growth plate in the elbow called the medial epicondylar physis.
Force along the inside of the elbow during throwing is more likely to cause failure at the area of the growth plate than at the UCL. This injury is often termed Little League Elbow. Reconstruction of the UCL may not be needed in this age group unless the injury to the UCL occurs after the growth plate is closed. Sometimes the ligament avulses or pulls away, taking a piece of the growth plate with it. When the condition has been present for some time, the ligament is not all that may be damaged. The entire elbow joint is at risk due to the abnormal forces caused by the repetitive stress injury.
 RSS-канал
RSS-канал
